This month, as we recognize both World Health Day (April 7th) and Earth Day (April 22nd), it’s the perfect time to emphasize the inevitable truth that we need to care for the Earth in order to care for ourselves and each other. Climate change is the single biggest threat facing humanity.

The World Health Organization estimates over 13 million deaths worldwide each year that are caused by avoidable environmental factors. The global crisis of climate change has already begun to affect public health: Over 90% of people breathe air contaminated by pollutants, and 13 per minute die of lung cancer, heart disease, and stroke (all highly exacerbated by unclean air). Microplastics can be found everywhere from the ocean floor to your lung tissue. Heat-related illness and fatalities are on the rise, and pre-existing energy grids are unequipped to handle these temperature extremes. Diseases spread more easily as mosquitos and other virus-carrying parasites thrive in warm conditions. Natural disasters such as hurricanes are highly exacerbated by the rising ocean temperatures. Already an average of 20 million people per year are displaced by extreme weather events. The right to breathe clean air, drink clean water, and maintain a nourishing diet are synonymous with the right to live, yet so many are deprived of these basic needs.
#HealthyClimatePrescription
At the 2021 United Nations climate negotiations in Glasgow, more than 600 health organizations representing over 46 million health workers published an open letter to heads of state and national delegations. The letter “prescribed” a course of treatment that must be followed in order to combat the growing threat that climate change poses to public health. The letter currently has over 5,200 signatures from medical health professionals in over 100 different countries. Not only did the letter enumerate the steps that governments must take in order to avert the future devastation promised by late-stage climate change, it also acknowledged precisely which populations must be held accountable and which populations are the most vulnerable:
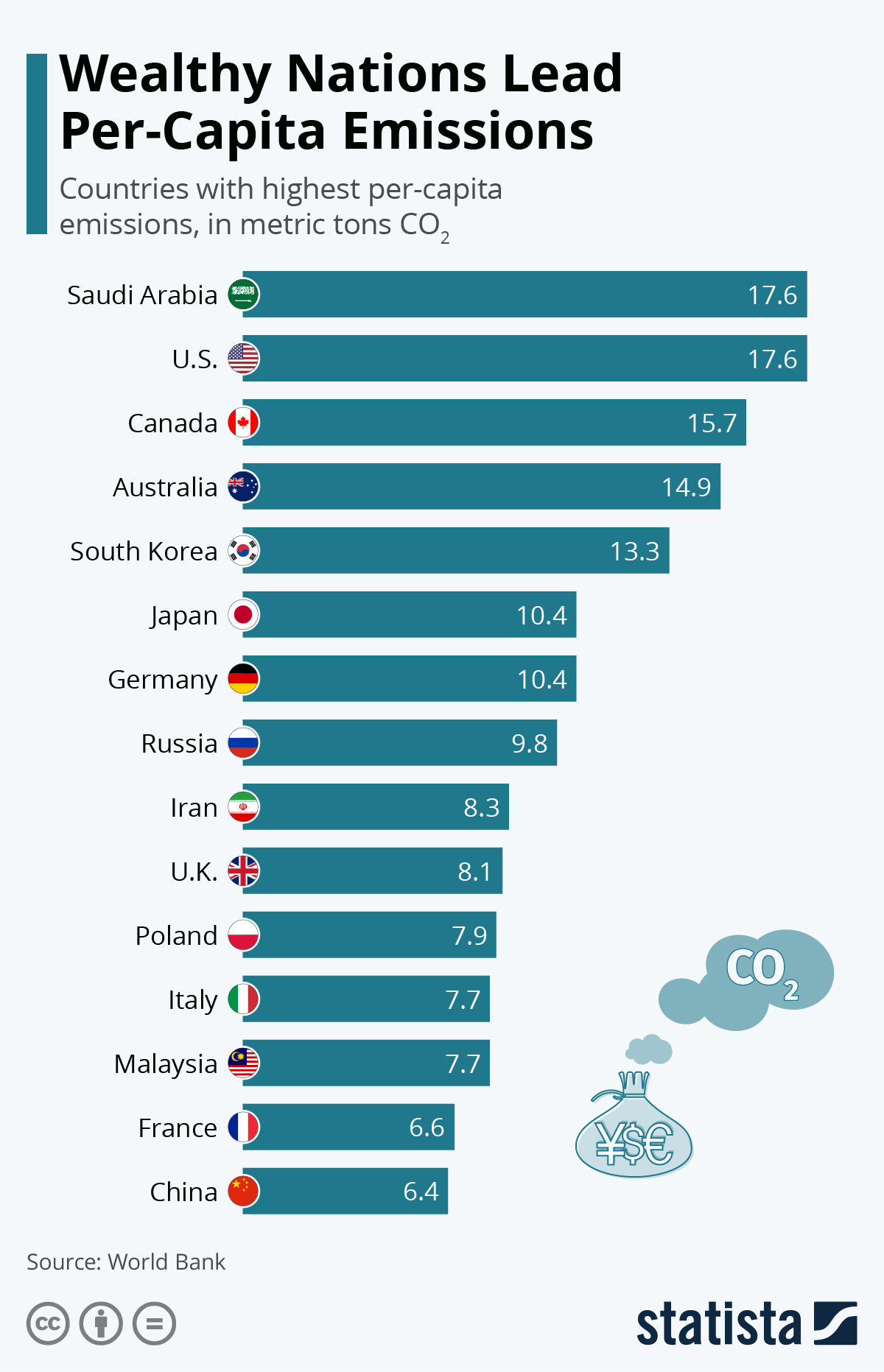
“While no one is safe from these risks, the people whose health is being harmed first and worst by the climate crisis are the people who contribute least to the problem and who are least able to protect themselves and their families against it—people in low-income countries and communities. Those people and nations who have benefited most from the activities that caused the climate crisis, especially fossil fuel extraction and use, have a great responsibility to do everything possible to help those who are now most at risk.
Integrating health and equity into climate policy will protect peoples’ health, maximize returns on investments, and build public support for the urgently needed climate actions. Cleaner air and water, healthier and more secure food supplies, a resilient, low-carbon health sector, and greener transportation and community design are all beneficial to people, here and now. Furthermore, the health cost savings will offset the costs of taking these actions.”
Click here to see view the letter in full and consider adding your signature.
Building A Climate-Resilient Health System
Remember the first months of the pandemic, when cars were off the roads and people were staying inside? Researchers found a dramatic decrease in heart attack incidents following this lifestyle shift. Stark data such as these indicate that we do have the power to make significant change in health outcomes—provided we are able to significantly change our reliance on fossil fuels and high-pollution practices.
What does a climate-resilient health system look like? According to the World Health Organization’s guidelines, there are four key pillars of sustainable health care.
The first is the health workforce itself: do your health employees have adequate working conditions? Are they “empowered and informed” to cope with environmental challenges? Are they, as people, in a place to be able to care for other people? In the wake of the pandemic, many health centers have found themselves lacking staff members as health practitioners struggle to maintain their physical and mental well-being. We lost around 20% of our health care staff due to the pandemic. In the future, we must find ways to better support hospital and clinic staff—applause is not enough.
The next important consideration for climate resiliency is water and hygiene. It is imperative that hospitals and health centers have access to clean water and sanitary supplies. Does your organization have reliable access to clean water? As of 2018, a full 50% of health care facilities worldwide lack piped water. Does your health center dispose of waste in a safe way? Proper sanitation is an important step in ensuring the future quality of environmental resources.
Energy access is the next domain to re-examine. Internationally, 59% of health care facilities lack reliable electricity. Has your organization considered transitioning to sustainable energy services? In the event of a power blackout, which we can expect to occur increasingly commonly, where will your organization find the energy to power x-ray machines, respirators, and even air conditioning?
Last but not least is infrastructure and technology. Everyone knows that keeping a facility safe is important, but did you know how many other improvements can be made in pursuit of energy efficiency? Painting your roof white, for example, can significantly reduce heat impact. Corridors and clinic exam rooms can be constructed to maximize natural light and ventilation. An on-site garden and a compost program can alleviate the environmental impact of wasteful hospital cafeterias. Medical equipment and supplies should be purchased locally, whenever possible. Modern laundry machines and dishwashers use less water and energy than out-of-date ones. Health care facilities must understand that initiating these climate-friendly adaptations today can help mitigate the anticipated climate emergencies of the future.
For more detailed suggestions on creating environmentally stable health facilities, click here.